SOAP notes document details from patient visits and let you communicate vital information to other healthcare providers. Download them for free from the websites mentioned in this article.

If you’re in the medical field, you already know how time-consuming taking patient notes and charting can be. Medical records have to be documented accurately and in an organized way so it’s easy to track patients’ progress and avoid miscommunication. For that purpose, most healthcare providers like you use SOAP notes.
SOAP notes let you record a patient's initial assessment, diagnosis, and treatment details in a standardized format, which can also be shared with and used by other healthcare providers.
If you’re new to SOAP notes, read on to learn what they are and how they can help standardize patient documentation. And if you already use them, we’ve got some free SOAP notes templates you can try. We’ve also suggested some popular medical software tools that offer built-in SOAP note templates.
What are SOAP notes and their benefits?
A subjective, objective, assessment, and plan (SOAP) note is a common documentation method used by healthcare providers to capture and record patient information, from the intake form and diagnosis to the treatment plan and progress notes. All SOAP notes have a standardized format that is divided into four categories (which we'll go over in the next section).
By organizing patient records in a defined template, these notes help cut down manual errors and miscommunication. Each piece of information is entered into a specific field on the template, so medical providers know where exactly to find the information they need. They don’t have to go through the entire form to find the one tiny bit of information they require.
A standardized SOAP note template also makes it easier to share records with other healthcare providers, if required. Since both use the same documentation method, there’ll be no miscommunication regarding a patient’s treatment plan or health status.
4 components of a SOAP note

1. Subjective
This covers your patient’s detailed medical history and current symptoms. Notes from your verbal interaction with patients as well as what they tell you about their condition go here. Record your patient’s chief complaint, existing symptoms, and any pain description in this section. Any comments, concerns, or questions your patients may have are also included here.
2. Objective
This is a record of your physical examination of the patient’s condition. It includes observations that can be measured such as body temperature, pulse rate, and blood pressure. It has details of any visible symptoms such as changed skin color or any abnormalities you feel when physically examining the patient. You can also include details of previous diagnostics tests (e.g., X-rays) and lab reports.
3. Assessment
The next component of a SOAP note is assessment. It includes a summary of your diagnosis of the patient’s existing condition. For any patient, there may be one clear diagnosis or multiple issues that require separate diagnoses. There may also be cases where a definitive diagnosis is not made by the physician, therefore many possible diagnoses are included in the assessment.
4. Plan
The last component of a SOAP note is the plan. It includes the treatment plan (e.g., medication, therapies, surgeries) you’ll follow for the patient. It may involve more tests to either confirm or rule out a diagnosis. The plan may even include details on the patient’s self-care, such as bed rest, days off work, and healthcare and lifestyle recommendations.
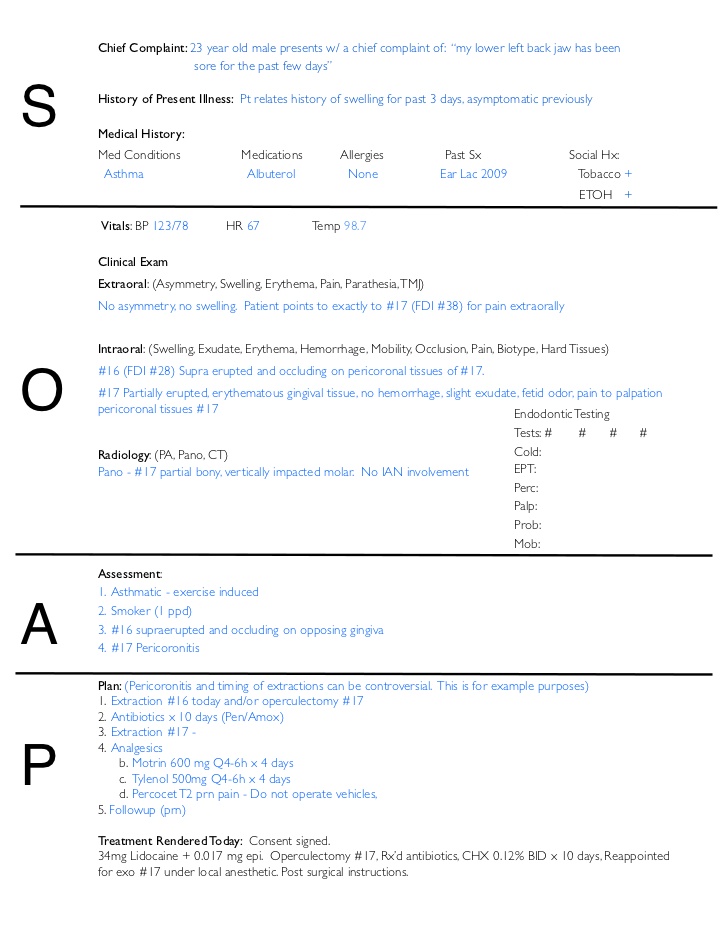

A sample SOAP note used in a dental practice (Source)
Free SOAP notes templates
Template Archive, SampleTemplates, and Safety Culture are three websites that offer free SOAP notes templates. These templates are fully editable so you can easily make changes to them.
Template Archive: This website offers over 30 free SOAP notes templates for medical specialties including psychiatry, asthma, psoriasis, pediatric, and orthopedic. The templates are available in PDF format and the file size starts from 15KB.
SampleTemplates: This website offers free SOAP notes templates related to nursing, physical therapy, pediatric, massage, clinical progress, and more. The formats for downloading the templates are DOC and PDF and the file size starts from 8KB.
Safety Culture: This website offers free SOAP notes templates for pediatrics and nursing. The templates are available as PDF files and the size starts from 14KB.
Medical software tools with built-in SOAP notes templates
If you’re willing to invest, there are specific medical software systems that offer built-in templates. With built-in SOAP notes, all patient records you enter are directly linked to and saved to your medical software.
We’ve listed the top three software tools that have SOAP note templates. These products are selected from Capterra’s electronic medical records software directory and listed alphabetically. Read our complete product selection methodology here.
75Health
75Health is cloud-based electronic health record software for medical practices of any size. The platform helps you keep up with medical records with the assistance of built-in SOAP notes templates. 75Health’s templates are designed to be used for discharge summaries, clinical notes, and consultation notes, and they are fully configurable so they can be tailored to fit the unique needs of your practice.
You can also use 75Health to schedule appointments, manage billing and invoices, submit insurance claims, and complete initial assessments for patients with the help of a standardized form.
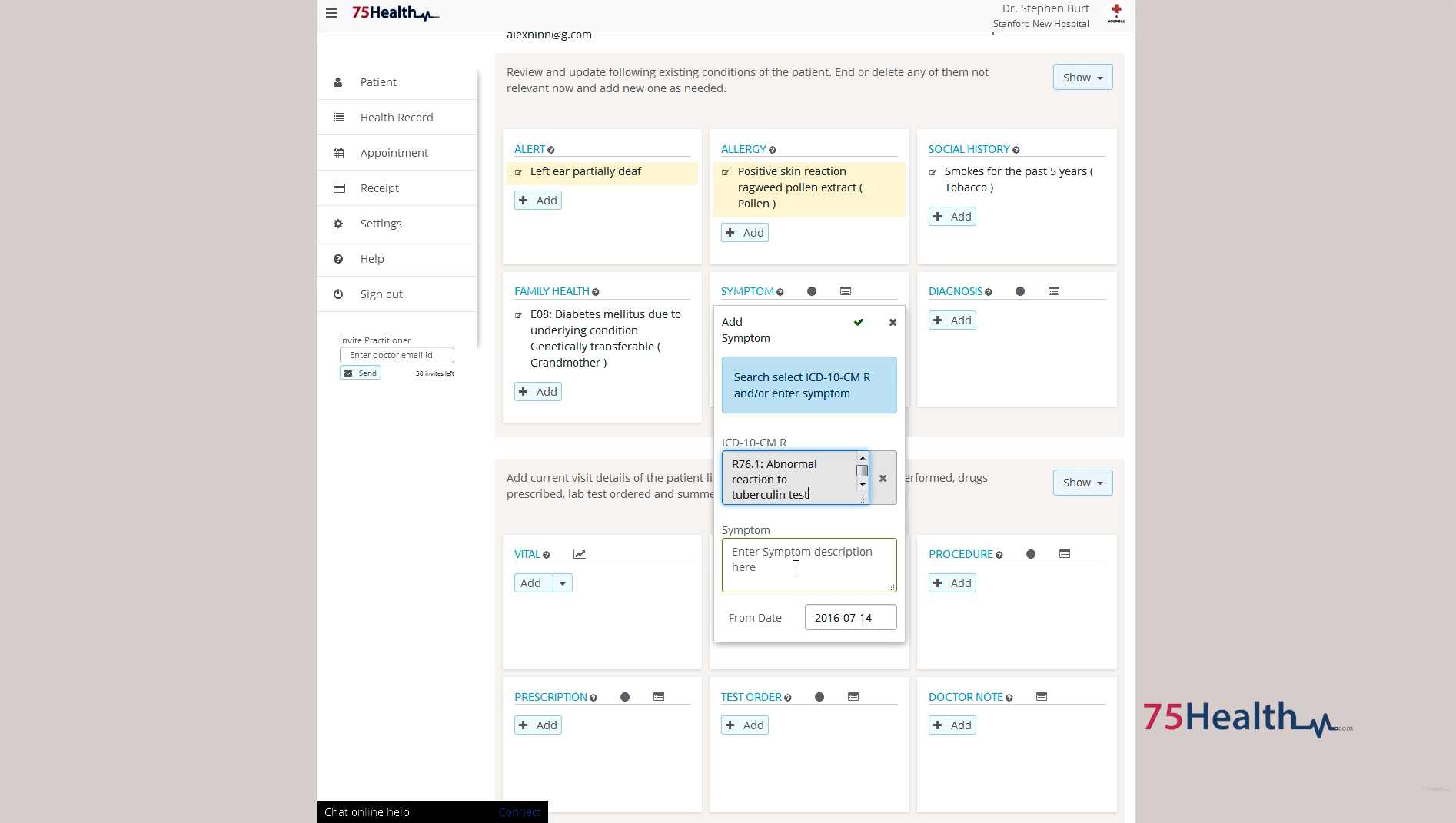
Updating a patient profile in 75Health (Source)
75Health starts at $19 per user, per month and includes unlimited patients and unlimited medical records charting. Before committing, make sure to take advantage of 75Health’s 14-day free trial.
CareCloud
CareCloud is cloud-based medical billing and electronic medical records software for practices of all sizes looking to improve productivity, profitability, and patient care. CareCloud has free SOAP note templates available for download, and they also have an electronic version of the templates built into their platform.
You can also use CareCloud to schedule appointments, manage insurance claims, set up electronic prescriptions, and obtain patient records. Additionally, CareCloud also features patient engagement and clinical reporting tools that allow you to drive better patient outcomes.

A downloadable SOAP note template from CareCloud (Source)
Pricing information for CareCloud isn’t publically available. We recommend scheduling a demo of the platform to get a feel for the tool and its associated costs.
PracticeFusion
PracticeFusion is a cloud-based electronic health records platform for medical practices of all sizes in the U.S. PracticeFusion currently services over 20,000 medical practices in the U.S.
PracticeFusion’s platform includes templates for medical charts and SOAP notes. These templates are pre-built but customizable, so you can adapt them to include information fields unique to your practice.
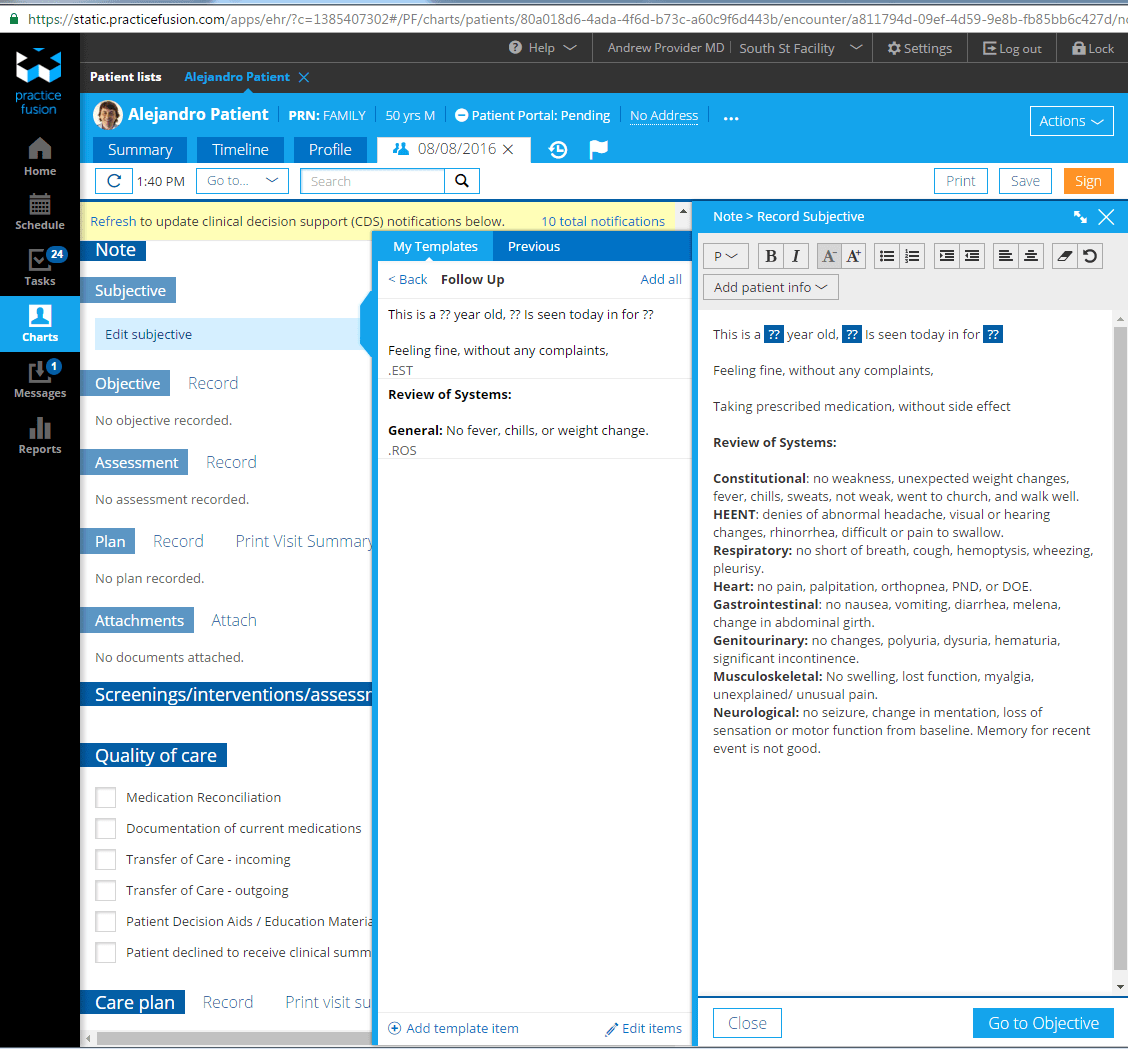
Recording a note for a follow-up appointment in PracticeFusion (Source)
PracticeFusion’s EHR starts at $149 per provider, per month and includes templates, e-prescribing capabilities, and free customer support. An annual subscription is required, but billing occurs monthly. PracticeFusion offers a 14-day free trial, so definitely give it a try before committing.
Start saving time with SOAP notes templates
If you already have EMR or practice management software that doesn’t offer SOAP notes, download them for free from the websites we’ve mentioned.
But if you’re looking to buy new software, we suggest opting for one that offers built-in SOAP note templates. You can select from the three tools we’ve recommended or check out more options on Capterra’s software directory.
